The friction points we see across providers, payers, and health-tech companies.

Fragmented patient data across systems
EHRs, billing systems, CRMs, and patient portals each hold a piece of the patient's record. Care teams make decisions from incomplete pictures — and patients feel it.

Multiple disconnected CRMs
Acquisitions, legacy implementations, and department-level tool sprawl leave organizations running two or three CRM systems simultaneously — with no single source of truth for patient or customer data.

Low adoption among clinical and admin staff
Salesforce implementations that weren't designed around real clinical workflows get bypassed. Data entry happens in arrears. Reports can't be trusted. Leadership flies blindly.

Compliance is treated as an afterthought
HIPAA, GDPR, and audit requirements added on top of a live Salesforce org after go-live. They create friction without actually reducing risk because they weren't architected in from the start.

Manual subscription & billing workflows
Health-tech companies managing subscription services, recurring billing, and service packages still rely on spreadsheets and custom scripts — with month-end close taking days instead of hours.

Integration backlogs block care delivery
EHR, EMR, medical device, and third-party platform integrations sit in backlog for months because the implementation partner didn't have the engineering depth to build and maintain them.
We build differently for providers, payers, and health-tech — because the priorities are genuinely different. Select your segment below. Many healthcare clients span multiple, and we scope accordingly.
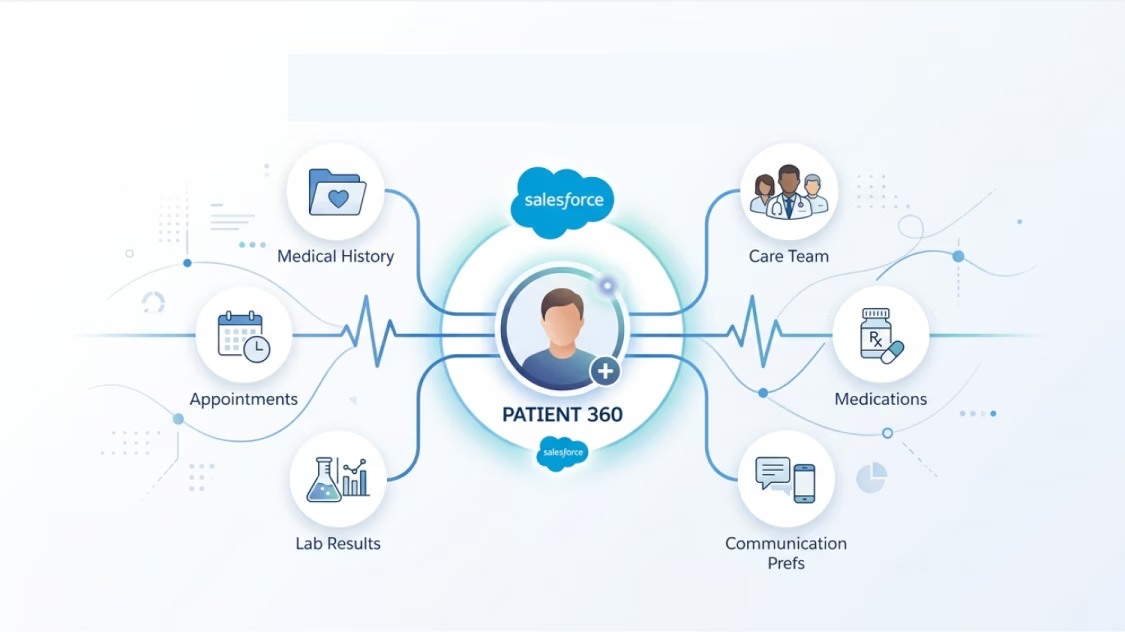
We implement Salesforce Health Cloud to build unified patient profiles that pull clinical and non-clinical data together — medical history, care team assignments, appointments, consent records, and communication preferences — so every interaction starts with a complete picture, not a fragmented one.
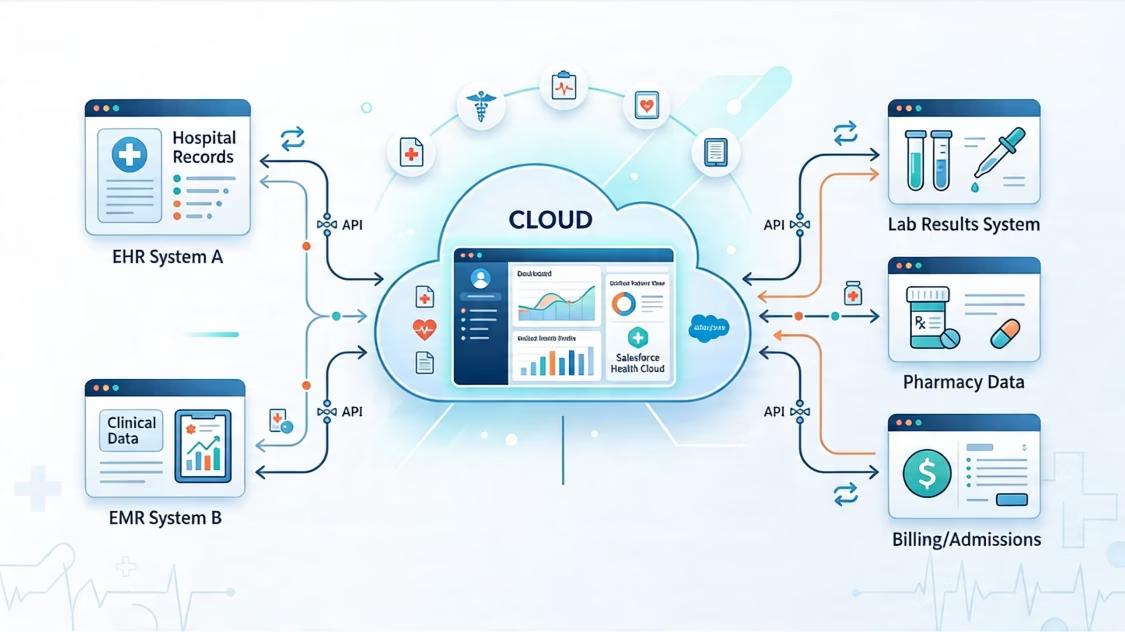
We connect Salesforce Health Cloud with EHR and EMR systems — including Epic, Cerner, Allscripts, and others — using FHIR-aligned integration patterns, enabling clinical data to flow into Salesforce in real time. Care teams stop switching between platforms and start making faster, better-informed decisions.

We build HIPAA-compliant patient portals on Salesforce Experience Cloud — appointment scheduling, care plan access, secure messaging, document upload, and case status tracking. Patients manage their own journey. Inbound call volume drops. Staff focuses on care, not admin.

We configure Salesforce Service Cloud to route patient interactions from web forms, calls, email, and chat into a unified queue — with intelligent case assignments, SLA timers, and escalation paths. Every channel feels consistent with the patient. Nothing falls between platforms.

We build structured referral workflows in Salesforce, so care transitions between departments, specialists, and external providers are tracked, acknowledged, and followed up on—not lost in email chains. Referral leakage drops. Continuity of care improves across every handoff.
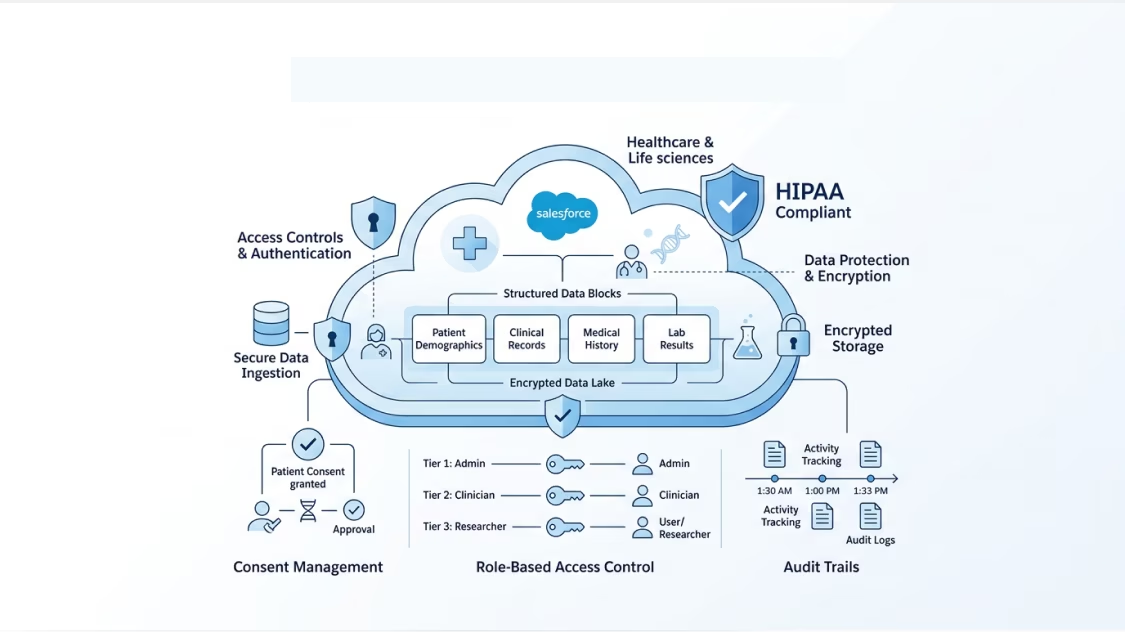
We architect Salesforce for healthcare from the ground up — field-level encryption for PHI, consent management, role-based access, audit trails, and data retention policies aligned to HIPAA and GDPR requirements. Compliance is built into the foundation, not layered on later.
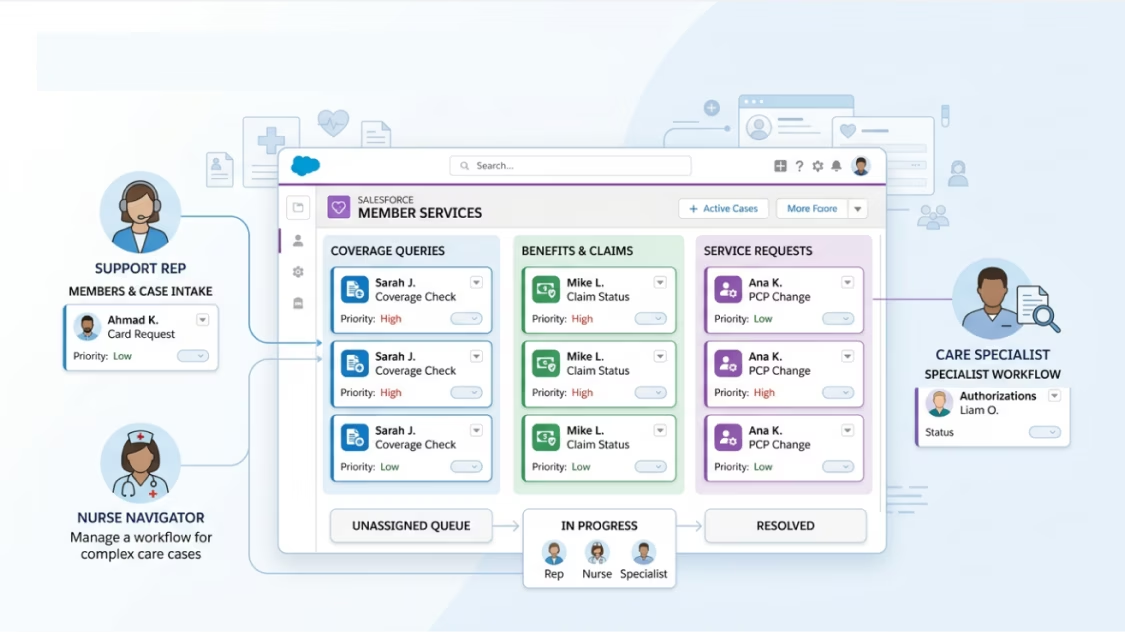
We configure Salesforce as the central engagement layer for member services — coverage queries, benefit explanations, and service requests — all routed and resolved within one platform. Customer service reps, utilization management nurses, and appeals specialists each get the workflows they need, not a generic case screen.
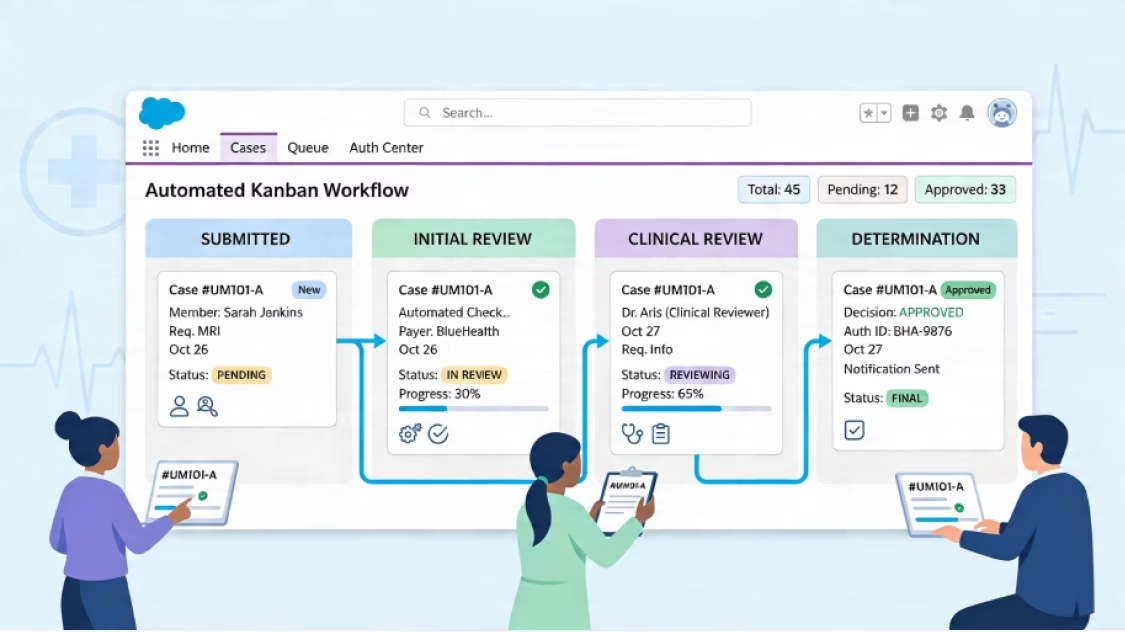
We automate authorizations in Salesforce, reducing manual work and providing real-time transparency into case status for all teams'.

We implement structured A&G case workflows in Salesforce Health Cloud — intake, classification, assignment, regulatory timelines, and resolution documentation — so appeals are handled consistently, compliantly, and with a full audit trail. No more cases are managed in shared inboxes.
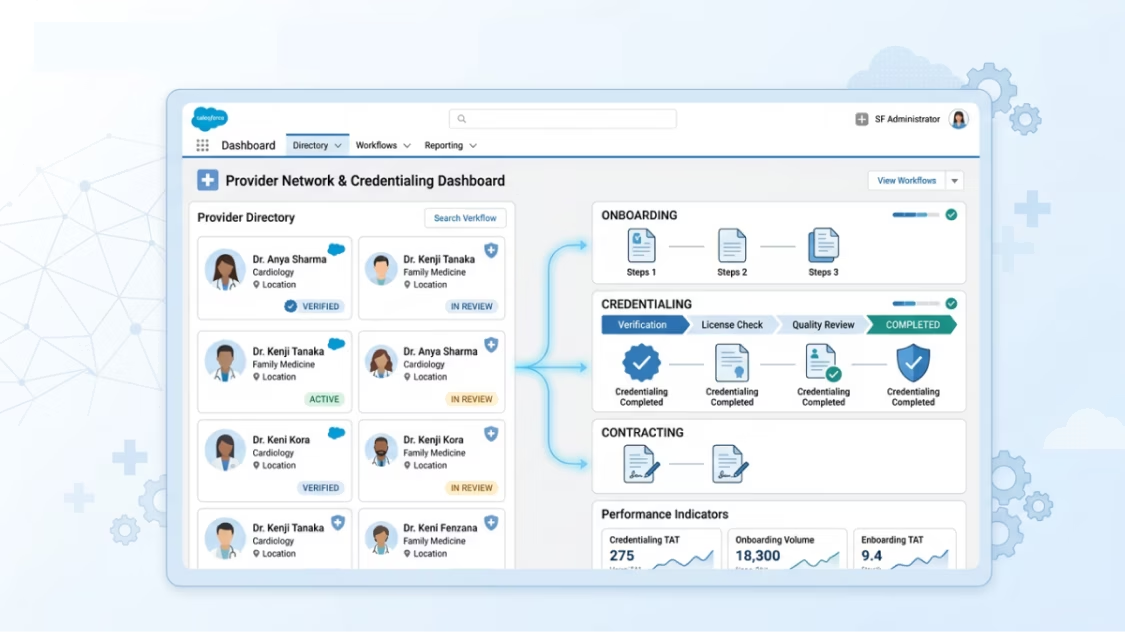
We build provider directories, onboard workflows, and credentialing processes inside Salesforce — so network management teams track provider status, contract terms, and performance data in one place. Provider relations stop living in spreadsheets and start being data driven.

We configure Marketing Cloud and Einstein AI within Salesforce to drive proactive member engagement — preventive care reminders, gap-in-care alerts, and personalized communications based on health plan, chronic condition, or utilization history. Outreach that's relevant gets responded to.
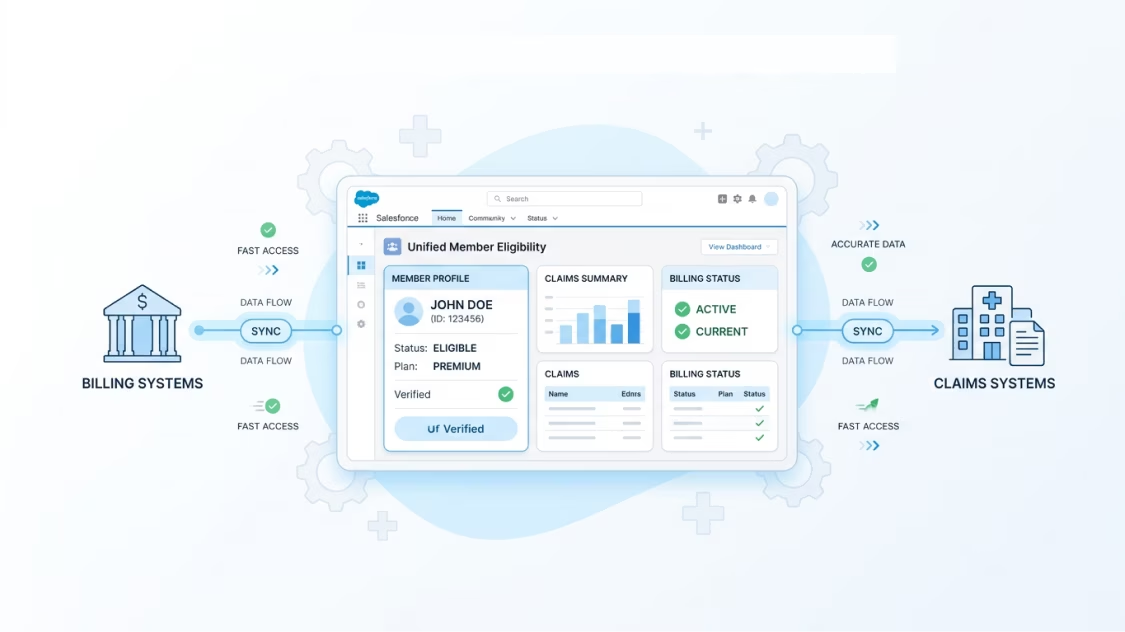
We integrate Salesforce with your claims processing and billing systems, so member services reps see accurate eligibility, claims history, and benefit details without leaving the platform. Faster answers for members. Fewer escalations for your team.

Health-tech Client
A health-tech company managing eFax subscription services was spending 4–5 days each month on manual invoicing. Their generic sales process couldn't accurately handle recurring subscriptions and one-time service combinations. We implemented Salesforce CPQ to automate pricing, quoting, and invoice generation — cutting quote turnaround time by 12% and eliminating the month-end manual crunch entirely.
Outcome → 12% faster quote turnaround, month-end close automated

Healthcare SaaS Client
We unified Microsoft Dynamics and legacy Salesforce into one org—migrating, deduplicating, rebuilding workflows, and integrating commercial tools for consistent data and adoption.
Outcome → Single source of truth, higher adoption, cleaner data

Healthcare Provider Client
A digital healthcare provider needed to bring patient cases, FAQs, chat support, and document management together on one platform — while connecting to their EMR and financial systems. We implemented Salesforce Health Cloud with a patient portal, chatbot, integrated messaging, and full EMR and billing system integrations. Staff stopped switching platforms. Patients got consistent, trackable service across every channel.
Outcome → Unified service layer, EHR-connected patient profiles

We're not Salesforce consultants. We're your engineering partner
Compliance requirements, integration complexity, and the stakes of patient data make healthcare one of the hardest sectors to get right with Salesforce. We have the engineering depth and testing rigor to do it properly.
HIPAA-first: Consent management, PHI encryption, audit trails, and access controls designed into the architecture from day one — never retrofitted.
Integration-deep: EHR, EMR, billing, medical devices, and third-party platforms — we connect what clinical and operational workflows actually depend on.
QA-rigorous: 30+ automation testing specialists validate every healthcare Salesforce build — functionally, for compliance, and under real integration conditions before go-live.
Migration-proven: We've consolidated fragmented CRM environments into clean, unified Salesforce orgs — with zero patient data loss and minimal disruption to live operations.
One promise: Salesforce that fits your business.
09
Industries
200+
Implementations
One partner, all clouds. Our expertise ensures each Salesforce product delivers maximum ROI.


We implement Salesforce CPQ for health-tech companies handling subscription services, recurring billing, usage-based pricing, and bundled packages — cutting quote turnaround times, eliminating manual pricing errors, and reducing month-end close from days to hours.

We consolidate fragmented CRM environments — Microsoft Dynamics, legacy Salesforce orgs, and custom tools — into one unified Salesforce instance, with full data migration, deduplication, workflow rebuilds, and third-party integrations. One platform. One version of every customer record.

We configure Salesforce for medical device, pharma, and medtech teams to manage HCP relationships — covering territory management, visit planning, sample tracking, engagement history, and next-best-action recommendations across field and digital channels.

We build patient support workflows in Salesforce covering intake, eligibility screening, enrolment, care coordinator assignment, adherence tracking, and renewals — so patient services teams spend less time on admin and more time on care.

We build Experience Cloud portals that extend Salesforce to distributors, healthcare facility partners, and patients — reducing support load through self-service and giving partners the visibility they need without direct system access.

Our 30+ automation testing specialists run functional, regression, and HIPAA-alignment testing across every Salesforce build — catching compliance gaps before production. EHR and billing system integrations are validated under real data conditions before go-live.
Health Cloud is built on top of Sales Cloud and Service Cloud and adds a healthcare-specific data model — patient and member profiles, care team structures, clinical data objects, care plans, consent management, and prebuilt HIPAA-ready workflows. Standard clouds require you to build all of that from scratch. For most healthcare providers and payers, Health Cloud is the faster, safer starting point. For health-tech and life sciences companies with primarily commercial use cases, Sales and Service Cloud with CPQ often makes more sense. We assess this honestly during a first conversation — the right answer depends on your workflows, not the price list.
We build compliance into the architecture from the start — not as a checklist item after go-live. That means field-level encryption for protected health information, role-based access controls aligned to minimum necessary standards, consent management objects that respect patient opt-outs across all channels, audit trails on every PHI-touching field change, and data retention policies enforced at the object level. Our 30+ automation testing specialists also run HIPAA-alignment testing before go-live to catch gaps before they reach production. Getting compliance right the first time is significantly cheaper than fixing it after patients' data has flowed through a non-compliant system.
Yes. We integrate Salesforce with major EHR and EMR platforms using FHIR-aligned patterns, and with billing and claims systems using MuleSoft and direct API connections. The scope and approach depend on which workflows you're launching first — we don't recommend integrating everything at once. A phased integration roadmap reduces risk and gets you live faster with the connections that deliver the most immediate clinical or operational value. We've also connected Salesforce with specialist platforms like 6sense, Pardot, Clearbit, and medical device data feeds in health-tech engagements.
Yes — CRM consolidation is one of our most common healthcare engagements. We've merged Microsoft Dynamics and legacy Salesforce orgs into a single unified instance, handling full data migration with deduplication, workflow rebuilds using Flows and CPQ, and integration reconnection for the entire commercial stack. The critical work is the data model design before migration begins — if the relationship and record structures aren't right, you just move the mess rather than fix it. We spend significant time on this up front so the migration lands cleanly.
A focused first release — patient or member profile model, care coordination workflows, case management, and core reporting — typically runs 8–14 weeks depending on data readiness and integration complexity. Health-tech implementations with CPQ and commercial workflows often move faster, in the 6–10 week range. Larger programs involving EHR integration, multi-site deployments, or full CRM consolidation are delivered in phased releases over several months. We define a phased roadmap upfront so clinical and operational value is visible at each stage, not just at the end.
All three — and our approach differs by segment because the workflows genuinely are different. Providers need care coordination, patient engagement, referral management, and EHR integration. Payers need member services, utilization management, prior authorizations, appeals and grievances, and provider network management. Health-tech and life sciences companies need CPQ for subscriptions, HCP relationship management, patient support programs, and often CRM consolidation following acquisitions. We ask about your segment and use-case priorities in the first conversation because they shape everything about how we architect and phase the engagement.
Low adoption in healthcare almost always traces back to a design problem — the system doesn't match how clinical or admin staff actually work. We address this before the build begins, not after go-live. We map real workflows with actual users, build role-specific interfaces and guided processes that fit daily habits, and avoid over-engineering screens that clinicians and coordinators will find confusing. We also track adoption metrics through dashboards post-launch and make targeted adjustments in the first 30–60 days when usage patterns show friction. Adoption is a delivery responsibility, not an afterthought.
Whether you're building a patient engagement platform, consolidating CRM systems, or automating a subscription billing workflow — we'll give you a direct, honest assessment of what's possible and what it takes.

Schedule a Free Strategic Call